Lockdown Hints and Tips for Heel Pain
During the Covid-19 lockdown there has been a large increase in the number of people taking up running as their choice of exercise, whether this be a new runner or an experienced runner running more frequently, resulting in an increase in people with painful heel conditions contacting the practice.
The heel is a specialised part of the body designed to absorb the impact of your body weight when walking, running or undertaking any other form of physical exertion or weight-bearing exercise. When pain does develop, it can be very disabling, making every step a problem, which in turn affects your overall posture.
Heel pain is common and is usually caused by small repetitive injuries that occur at a rate faster than the body can heal them. It can affect anyone but does seem to affect those who are middle aged, those who are overweight or stand for long periods of time due to work, as well as athletes. Heel pain can also be caused by lower back problems or inflammatory joint conditions, or simply due to the way your foot is functioning.
Although many people believe that their heel pain is “plantar fasciitis”, there are a number of other conditions that may be causing your heel pain including nerve entrapment, heel bursae, Haglunds bumps, Sever’s disease and Achilles tendinopathy.
You may ultimately need the intervention of a podiatrist to help diagnose the cause and resolve your heel pain. Here are some things you can do for yourself which may help or completely resolve your symptoms. Remember that heel pain can be a sign of an underlying problem and the cause itself may need investigating further to prevent recurrence.
Plantar fasciitis
This is caused by microtears in the fascia ‘band’ which connects the heel bone to the base of the toes, usually where it meets the heel bone. This condition can be caused by running, walking or standing for long periods of time, inadequate footwear or support, being overweight, overuse or sudden stretching of your sole, as well as a tight Achilles tendon.
There are often no visible features on the heel, but the pain is usually worse on standing after long periods of rest, particularly first thing in the morning.
Self care tips: rest your foot as much as possible and stretching exercises can help (see below). In the acute stage, use ice compresses for 10 minutes twice a day. Ensure you wear supportive footwear that is not completely flat.
In the long term orthotics may be prescribed to help the feet to function more effectively and help to make any possible recurrence less likely. Chronic cases which are not responding to an exercise regime often respond well to shockwave therapy. This is a highly rated treatment option for musculoskeletal tissues including tendons and ligaments. A high energy probe is applied to the area as acoustic waves are used to reduce pain and accelerate tissue repair and cell growth.
Tarsal Tunnel Syndrome
The tarsal tunnel is located on the inside of the ankle and is formed by the ankle bones and the band of ligaments that stretches across the foot.
Tarsal tunnel syndrome is similar to carpal tunnel syndrome, which occurs in the wrist. Both disorders arise from the compression of a nerve in a confined space. Tarsal tunnel syndrome is caused by compression of the posterior tibial nerve as it travels through the tarsal tunnel. Compression of the posterior tibial nerve can cause pain, tingling or numbness in the foot.
Symptoms are typically felt on the inside of the ankle and/or on the bottom of the foot. In some people, a symptom may be isolated and occur in just one spot. In others, it may extend to the heel, arch, toes and even the calf.
Sometimes the symptoms of the syndrome appear suddenly. They are often brought on or aggravated by overuse of the foot, such as in prolonged standing, walking, exercising or beginning a new exercise program.
Self care tips: rest and icing the area can help with any pain and inflammation. Supportive footwear will relieve pressure in the area.
Functional orthoses may be required to reduce the nerve compression. If these measures are insufficient, a steroid injection will often reduce the inflammation around the nerve. Occasionally a referral for surgical intervention is required.
Heel bursitis
This is an inflammation of a bursa (a fluid-filled sac) under the heel bone where the pain is typically more in the centre of the heel and gets worse throughout the day. This condition can be caused by a fall from a height on to the heel or over-use.
Pain can be felt at the back of the heel when the ankle joint is moved and there may be a swelling on both sides of the Achilles tendon. Or you may feel pain deep inside the heel when it makes contact with the ground.
Self care tip: a soft heel cushion can often help this condition.
Low level laser treatment or shockwave therapy may be helpful in long term conditions.
Haglunds bumps
These are firm bumps on the back of the heel, usually caused by excessive shoe rubbing in the heel area, or the thickening of the tissues associated with a tight Achilles tendon.
Self care tips: a small heel lift or other adjustments to footwear is usually enough to make them comfortable. A leather heel counter or wearing boots may help.
Haglunds bumps are often linked to high-arched or very flat foot types. Orthoses may help to reduce the excessive shear forces that are usually a factor in their formation. In more serious cases, surgery may be necessary.
Sever’s disease (calcaneal apophysitis)
This condition affects young children usually between the ages of 8 and 12, especially if they are physically active or undergoing a growth spurt. It results from tearing of the bone growth plate in the heel bone (calcaneus) where the Achilles tendon attaches to the heel.
This condition is temporary and self-limiting but can be distressingly painful at the time.
Self care tips: rest, ice packs and a small heel lift may help in the early stages. Stretching exercises may help but should be used later as part of the rehabilitation process.
Orthoses may be helpful in realigning the heel. A supervised rehabilitation programme is recommended as the right exercise at the right time is important.
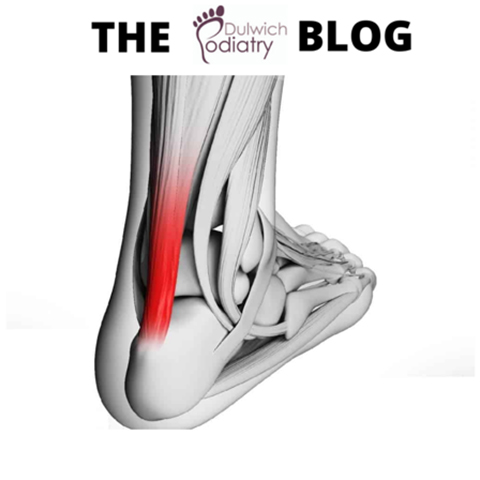
Achilles tendinopathy
When the Achilles tendon is placed under excessive strain, small tears can develop along with inflammation. In some cases a more major tear or even a rupture can occur.
Self care tips: rest, ice packs and gentle exercises may help in the early stages.
Treatment involves special exercises that strengthen the tendon and increasing the height of the heel with a heel lift or orthoses. Shockwave therapy is very effective where the problem lasts more than three months. Again, a structured rehabilitation programme will prevent recurrence of the problem.
Self care tips summary
If you experience heel pain:
- Minimise walking or exercising on hard ground
- Rest regularly and try not to walk or run too fast
- Wear a raised heel (no more than 6-10 mm higher than normal)
- Lose weight if you are overweight